Skip to content
‘It’s a Desperate Time’
The surge of coronavirus cases is crowding large metropolitan hospitals, putting pressure on smaller facilities
By Melanie Evans, Ian Lovett and Christine Mai-Duc / Photographs by Allison Zaucha for The Wall Street Journal
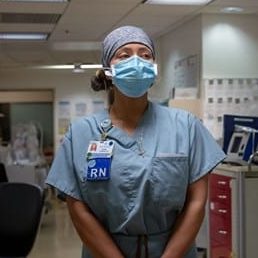 BALDWIN PARK, Calif.—On New Year’s Day at Kaiser Permanente’s medical center in this suburb east of Los Angeles, the overflowing emergency room spilled into the hallway. Doctors treated patients on oxygen in the waiting room after running out of beds. Some 80% of patients admitted in recent days have Covid-19.
BALDWIN PARK, Calif.—On New Year’s Day at Kaiser Permanente’s medical center in this suburb east of Los Angeles, the overflowing emergency room spilled into the hallway. Doctors treated patients on oxygen in the waiting room after running out of beds. Some 80% of patients admitted in recent days have Covid-19.
In Texas, patients who need to be transferred from small facilities to big metropolitan hospitals sit in limbo for hours or days, putting them at risk of developing complications from delays. Desperate smaller hospitals have flown patients as far as Albuquerque, N.M., and Oklahoma City for an open bed.
In North Carolina, rising numbers of intensive-care patients in Charlotte have forced doctors to save those beds for the “sickest of the sickest” from Covid and find somewhere else in hospitals for all other critically ill patients, one hospital official said.
Across the nation, the surge of coronavirus cases is crowding large metro hospitals with Covid-19 patients, pushing occupancy against the limits of space and overwhelming nurses and doctors. More than 40% to 60% of ICU patients in some metro areas are critically ill from Covid-19, according to an analysis of federal data by the University of Minnesota Hospitalization Tracking Project.
The crisis is a public-health threat that reaches far beyond major cities, say doctors, nurses, public officials and experts in health-care policy. The biggest hospitals in major metro areas often have specialists and lifesaving equipment lacking at smaller regional hospitals. They serve as a release valve when smaller facilities are overrun. As large hospitals fill, they close to local ambulances as well as most patient transfers, creating a far-reaching strain on regional heath-care networks.
“They’re all backed up,” said John Friel, chief executive of the 30-bed hospital in Big Bear Lake, Calif., two hours east of Los Angeles. The hospital has no ICU and is using its emergency room to hold critically ill patients, he said. An air ambulance flew one patient to Reno, Nev., for an open bed.
Surges in the spring and summer also slammed hospitals in metro areas, but were more geographically concentrated into hot spots. The latest surge is more widespread, said Eric Toner, a senior scholar with the Johns Hopkins Center for Health Security. Nationally, Covid-19 patients in hospitals reached about 123,600 as of Jan. 2, data from the Covid Tracking Project show, with more than 21,200 hospitalized in California. “What we’re seeing in California could happen in almost any other community in the United States in a matter of weeks,” he said.
Deaths nationally from the novel coronavirus have surpassed 350,000, according to Johns Hopkins University data.
Coming weeks are expected to further stress hospitals already in crisis, said doctors and public-health officials, with infections spread during holiday gatherings leading to more waves of patients in emergency rooms. “Many hospitals have reached a crisis point and are having to make many tough decisions about patient care,” said Christina Ghaly, director of the Department of Health Services in Los Angeles County, where Covid-19 deaths recently surpassed 10,000.
Los Angeles County has reported an average of 13,988 new cases per day for the past two weeks and infections appear to be increasing, based on the average during the prior seven days, Johns Hopkins University data show. The county’s daily average new cases is three times as many as any other U.S. county.
Three hospitals have notified California officials of plans to implement “crisis care,” or standards used to decide how to prioritize treatment when there aren’t enough resources to care for all patients. The California Department of Public Health said the “state immediately responded to mitigate the situation so that those three hospitals are not rationing or withholding care—and are no longer in crisis care mode.”
Doctors, two chaplains, a bioethicist and others met daily last week at the Methodist Hospital of Southern California to review intensive care and emergency room patients and available resources, but have not yet been forced to ration medical care, said the hospital’s spokesman, Clifford Daniels. “That committee would not be meeting if we didn’t see the potential need,” he said.
Hospitals urgently need staff, said officials, and are offering sizable bonuses to recruit new workers, asking retirees to return to the workforce and suspending some surgery to redeploy health-care workers from operating rooms to help out with other patients. Doctors and nurses are exhausted and anxious, they said, as they care for more patients.
As of New Year’s Eve, L.A. County health officials said they had vaccinated more than 11,000 front-line health-care workers.
Hospitals inundated by the surge are reporting shortages of critical supplies, including oxygen tanks for ventilators and sterile water, which is critical to safely operating machines that push air into the lungs.
“We ran out of beds last week,” said Chris Van Gorder, chief executive of Scripps Health in San Diego, which also asked the county for additional ventilators. A shipment of the machines he ordered in March arrived last week. The five-hospital system in late December got half its order of sterile water, as national demand exceeded supply.
“It’s a desperate time,” Dr. Toner of Johns Hopkins said. “This is what we have been warning about for a year now. If we let our hospitals get overrun, we’re going to see a lot more deaths, not only among Covid patients, but heart attacks and strokes.”
At Kaiser Permanente Baldwin Park Medical Center, the crush of Covid patients has left almost no space in the emergency department. Offices have been converted into exam rooms and many non-Covid patients are sent to a tent outside.
An entryway between two sets of sliding doors had been repurposed as a space to treat people who came in by ambulance and needed emergency care before it was possible to determine whether they had Covid.
“We have patients waiting 12 hours to get seen. A lot of patients give up and go home,” said Dicky Shah, assistant chief of the emergency department at Baldwin Park Medical Center. “It feels like we’re in wartime.”
Baldwin Park is part of the corridor east of Los Angeles that’s been pummeled by Covid-19. A working-class city of 75,000 people, 75% of its residents are Latino. Overall in Los Angeles County, Latinos are contracting the virus at more than twice the rate of white residents, according to data from the county, in part because they are more likely to be essential workers and to live in more crowded homes.
On New Year’s Day, Los Angeles county public-health officials reported 20,414 new daily cases, another record, and 207 deaths. More than 7,600 people in the county were hospitalized with Covid-19, with more than 1,590 of those in intensive care units.
At Baldwin Park Medical Center, the overcrowded ICU has meant emergency room doctors must raise the bar for who they admit, sending some home they would have typically kept, Dr. Shah said.
“We don’t have a choice,” he said. “Our hospital is so full that we’ve started admitting only patients once they’re really sick.”
The hospital, which can typically manage 150 to 160 patients, has held more than 200 patients in recent weeks, said Ramin Davidoff, executive medical director of the Southern California Permanente Medical Group. “What we’ve tried to do is to prepare for absolute worst-case scenarios,” he said. “We’re right at that worst-case scenario.”
The hospital has rapidly expanded to four intensive care units from one, and pulled nurses from across Kaiser to work in ICU teams, allowing nurses to care for more patients. The strategy hasn’t compromised care, Dr. Davidoff said.
The staffing changes, rapid expansion and makeshift units have distressed some staff. Silvia Espinoza, a full-time ICU nurse, worked her first shift in an ad hoc unit Friday, starting at 3 a.m. She was still at work 15 hours later.
“It’s terrible,” she said. “We don’t have the proper staff. We don’t have the proper equipment. Our doctors are not here all the time because we now have three different ICUs.” As a result, she was constantly running back and forth to the regular ICU to get supplies like rapid infusers and saline flushes, she said.
Staff propped doors open on the makeshift unit, allowing them to see into rooms but also allowing air to flow. Filters in patient rooms worked to suck air outside from contagious patient rooms.
Ms. Espinoza said she works alongside nurses deployed from elsewhere in the hospital and cares for a growing number of patients. “It’s actually very dangerous, because they go into a panic. They don’t know what to do,” she said of working with nurses not accustomed to the ICU. “One ICU nurse should have max two patients. That’s not happening. We have three. Now they’re telling us they’re going to give us four.”
In a statement, the hospital said it has had to move to a team-based nursing approach during the surge, “which means that each patient actually has a larger clinical team assigned to them.”
The staffing shortages have been the toughest to manage, Dr. Davidoff said. Kaiser Permanente is able to transfer patients across its 15 hospitals in Southern California to relieve strain on those hardest hit by the pandemic. The hospital has a better supply of personal protective gear for workers than it did in the summer, he said, and has enough ventilators.
Across Los Angeles, hospitals have been pushed to their capacity. Cedars-Sinai has halted 80% of scheduled procedures to free staff and space for coronavirus patients, helping to increase its ICU capacity by 50%, said Jeffrey Smith, its chief operating officer.
Yet Cedars-Sinai, which includes one of the largest hospitals in Los Angeles County, has stopped accepting transfers except those required under federal law. “Our ability to take those now is really limited to the emergent cases,” he said.
About 90 minutes east of Los Angeles, Mountains Community Hospital now largely cannot transfer patients to larger hospitals for intensive care. “Every once and a while, I can pull a string and get someone really, really critical out of here, but that’s few and far between,” said Terry Peña, the hospital’s chief nursing officer and chief of operations.
The small hospital has 17 beds, and added three in a conference room on New Year’s Eve. It has no intensive-care unit. A metal construction trailer in the snowy hospital parking lot now doubles as a morgue. On New Year’s Day, the hospital had 11 patients in an emergency room designed for about half that number.
Ms. Peña, who had time only for a handful of one-hour naps the night before, reviewed applications she received overnight after the hospital made a New Year’s Eve plea on Facebook for nurses, including students, paramedics and emergency responders.
“We are experiencing a sudden surge of COVID cases in our community and temporary help is urgently needed,” the post said. Covid-19 cases have been rising since November, Ms. Peña said, but lately soared. The hospital is located in mountainous Lake Arrowhead, Calif., and the local population swelled in the pandemic, as many fled there to live and work remotely.
Her staff is exhausted, she said. “They will work themselves to death,” she said. “Everybody’s trying, but they are burning out fast.”
Delays have forced hospitals to look across state lines. In Hereford, Texas, the Deaf Smith County hospital is transferring patients to Albuquerque and Oklahoma City, with no beds available in nearby cities, including Dallas, said Jeff Barnhart, chief executive officer of the county hospital district.
“It’s all about just trying to find a bed,” said Mr. Barnhart, who is also an emergency medical technician and who has joined ambulance crews for emergency calls and patient transfers during the pandemic. His 42-bed hospital has had to turn down transfer requests from smaller hospitals, which it had typically accepted.
The longer search for fewer open beds, a largely manual process in many states that requires dozens of phone calls, increases risks for patients left waiting, doctors said.
Baylor Scott & White Health has 51 hospitals in Texas. Its nine hospitals around Dallas and nearby Fort Worth are now turning down some transfer requests, asking outlying hospitals to try again in 12 hours, said Alejandro Arroliga, Baylor Scott & White’s chief medical officer.
As critical patients wait in limbo for hospital beds, their condition often becomes worse, Dr. Arroliga said. “When you get transfers late, the patients tend to come in worse condition.” The system has seen its Covid-19 patients soar 55% higher than its last peak in July.
In North Carolina’s Mecklenburg County, ICUs for adults were 94% full in the week before Christmas, an analysis of federal data by the University of Minnesota Hospitalization Tracking Project shows, with half occupied by Covid-19 patients.
Katie Passaretti, medical director of health system infection prevention at Atrium Health, which includes one of the largest hospitals in Charlotte, N.C., said, “Now, it really is becoming everywhere that only the sickest of the sickest are in the ICUs.”
Kim McGuire2026-03-26T15:26:45-07:00
Page load link
 BALDWIN PARK, Calif.—On New Year’s Day at Kaiser Permanente’s medical center in this suburb east of Los Angeles, the overflowing emergency room spilled into the hallway. Doctors treated patients on oxygen in the waiting room after running out of beds. Some 80% of patients admitted in recent days have Covid-19.
BALDWIN PARK, Calif.—On New Year’s Day at Kaiser Permanente’s medical center in this suburb east of Los Angeles, the overflowing emergency room spilled into the hallway. Doctors treated patients on oxygen in the waiting room after running out of beds. Some 80% of patients admitted in recent days have Covid-19.